The mental health of the global healthcare workforce is suffering. With 93% of healthcare workers stating they are experiencing stress, and as many as 86% reporting they are experiencing anxiety, it is time for healthcare leaders to act.
All the world’s a stage and all the men and women are merely players. I am not a huge Shakespeare enthusiast, but this opening line keeps running through my head; I’ll explain why in a minute. But first, a few weeks ago I had the privilege of attending the Replenishing Yourself, Your Team, and Your Organization event hosted by Healthcare Plus Solutions Group. There were numerous meaningful topics, but one stood out to me above all others – healthcare organizations need to prioritize mental health.
Which brings me back to Shakespeare: hospitals, doctor’s offices, urgent care clinics etc. are the stage, and for too long, healthcare workers have been seen as merely players. But we are not characters in a play – we are real people who witness trauma, feel fear, and who physically and mentally give of ourselves until we have nothing left. It’s time to stop looking at our healthcare workforce as cogs in a wheel, but actual people who are in desperate need of mental health support.
Katie Boston Leary, who leads ANA’s Healthy Nurse Healthy Nation initiative, provided tips for organizations to shift their focus back to the players of their organizations and make mental health a thing (her words, not mine).
Top eight ways organizations can start to do just that: Make Mental Health a Thing!
1. Include in the strategic plan for continuous and intentional focus and funding
Mental health resources cost money, which means leaders at all levels need to budget funding for meaningful programs. Popular author and podcaster Malcolm Gladwell theorized that you need 10,000 hours of practice in any particular area before you are deemed an expert. Providing a 10-minute CBL or one hour self-care course is not cutting it. We have to plan for and equip our workforce with tools they need to support their mental wellbeing.
2. Develop white flag language to indicate when people are not okay
Oftentimes, as leaders, we may not feel equipped to identify when our workers need help. To many of us, they might seem okay – and let’s face it, we’ve probably all been guilty of using language carelessly so that our peers and colleagues would have a difficult time knowing the extent of our challenges. White flag language is a way for leaders and their teams to communicate when someone is struggling beyond normal tiredness or stress.
3. Managers need to be vulnerable and authentic
Many leaders think we have to be stoic or we will be seen as weak. This is not true. Trust is established when leaders are vulnerable. Vulnerability leads to more trust and feeling safe. Your authenticity and honesty about your own struggles creates a culture where others can do the same.
4. There should be a bank of hours to accumulate and utilize for mental health days off
This one doesn’t need much explanation. Typically we require our workforce to provide advanced notice for time-off with the exception of when they are physically ill.
If someone needs a day off because they are experiencing a mental health struggle, we should give it to them. It’s pretty simple.
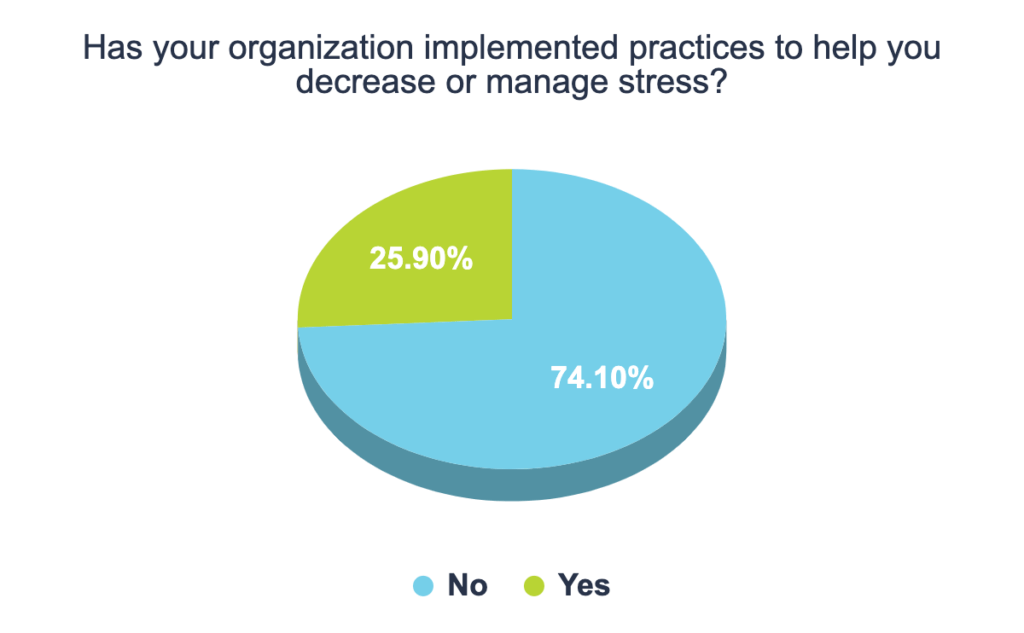
Matchwell surveyed a group of 500 nurses and found that most organizations are not implementing programs to help with stress and mental health.
5. All managers should be upskilled to manage conversations on mental health
Upskilled simply means that we need training too. Leading conversations around mental health is not in a general leadership job description nor is it a part of most leadership training. We can’t expect our employees to be experts on having these hard conversations if their leaders aren’t trained.
6. Treat employees like customers – staff satisfaction is equally as important as patient satisfaction
Over the last few decades patient satisfaction/patient experience has been the main focus for healthcare organizations. However, the satisfaction of our employees is just as important if not more so because if our workforce isn’t well our patients will suffer. Data show that organizations with high levels of burnout and fatigue have higher rates of hospital-acquired infections, medication errors, and even death. The mental health of our workforce matters.
7. Continually assess and measure mental health and wellness
A practical tool Katie Boston Leary recommends is the Staff Wellbeing Tracker. The staff fill it out for each shift, and it can be one way for leaders to monitor the wellbeing of their workforce and to know when to jump in to assist. There are three categories:
Good Shift (felt supported by the team)
Average Shift
Stressed Shift
At the end of each shift, nurses and other support staff can quickly complete the tracker and it gives leaders a way to quantify perceived stress.
8. Leaders must model the behaviors for the teams they lead!
Practice what you preach. I think Stephen Beeson says it best –
Your Call to Action: Determine who you want to be… and act to be that person. Repeat…
As healthcare leaders, we need to remove the stigma from mental health so that our workforce can get the help that they need. Historically, healthcare is a stoic profession, and workers are seen as weak if they can’t handle or manage the stress. Mental health needs to be a priority in healthcare.
What Do You Think?
What’s your experience with mental health as a healthcare professional? Please comment on this blog or share on social media. Together we can define ways to encourage more people to begin and continue meaningful careers in healthcare.

